At age 36, Dionne Nesbeth was diagnosed with diabetes, and months later she experienced two heart attacks that resembled a case of indigestion.
“I started feeling chest pains and thought it was indigestion. I didn’t take it as anything because at 36, I told myself I am too young to have a heart attack,” the Heart Smart Centre Wear Red ambassador, who speaks on behalf of the many women beset with heart disease in Jamaica, told a gathering during a reception earlier this month.
In fact, instead of visiting the doctor after fainting, Nesbeth said she decided to rest because she felt her condition was caused by something she must have eaten. She even drove herself home after the fainting subsided, because, again, “At 36, I couldn’t be experiencing a heart attack” she convinced herself.
It was not until she started having some serious chest pains and numbness in her left arm that she decided to check it out.
Nesbeth’s case is not unique says cardiologist Dr Claudine Lewis, but the disbelief she experienced may have been bolstered by the images portraying heart disease. “The images advertising heart disease is usually a man holding his chest,” she states.
Her aim is to raise awareness among women that this is something that affects them equally. “And not just heart attacks, we are talking about every single kind of heart disease, which is not discriminatory as it relates to gender or age,” she argued.
“You have heart disease from you are born, all the way up to a child … . We talk about living healthy lifestyles, and must remember that there are heart conditions that we have no control [over]. A rhythm abnormality, for instance, is not something you can eat yourself out of,” said Dr Lewis.
However, these are things that can be picked up early with a screening test, said the cardiologist, who argues that there is not enough information about heart disease in women, unlike the efforts placed in building awareness around breast cancer, for example.
Dr Lewis says she is prone to heart disease because of her strong family history and high cholesterol, although she is slim, so she does routine screening.
She was able to get three of her patients, Nesbeth, Venetta Smith-Bowen and P.J. Stewart, to become Heart Smart Centre Wear Red ambassadors during the week leading up to February 3.
HEART ATTACK MISTAKEN FOR GAS PAINS
Smith-Bowen, at age 33, thought she was having gas pains so she drank tea. However, she became concerned quicker than Nesbeth and decided to visit the doctor, who did an electrocardiogram (ECG) and found abnormalities. “He referred me to do an echocardiogram, which I did. during that test it showed I had a leaking valve in 2011.”
She said she went about her business normally, because for her the idea of doing surgery was a “no-no”.
In 2020, she started feeling pain in her stomach, back, other parts of her body, except for her chest. “Weakness in the legs, sometimes swelling, and back and forth to the doctor,” said Smith-Bowen.
She decided to go overseas to spend time with her sister, and while home alone she passed out. When her sister found her, she was conscious but weak. By the time she got to the hospital her situation had worsened, and while doctors were doing a test she passed out again and went into a coma.
Her sister signed for the surgery she never wanted to do all these years. She was unconscious for six days.
Today, at 45, her lifestyle has changed. Her eating habits have changed, and she now walks three miles in the mornings. Before, she would walk and tire. “Two heart valves were leaking, they replaced one and they repaired the other. If you come close to me sometimes you can hear one going tick, tick, tick, tick,” she quipped.
Smith-Bowen can laugh today about her condition because she is far more aware, and she is on heart-saving medication.
Nesbeth says she was referred to Dr Lewis, who told her that life did not stop because she had two heart attacks. “I was fretting. I was fearful, because I have heard so many stories of people not living through heart attacks. But Dr Lewis told me that the treatment you receive right after a heart attack is very important.”
She has done an angioplasty, which is where doctors open the arteries with a stent to allow blood flow.
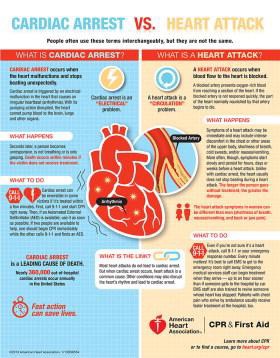
A heart attack is a blockage of one or two arteries inside the heart restricting blood flow.
She admits it has not been easy changing her diet, but gradually the body becomes in tune with the person eating better.
Both women take several pills to stay alive as well, and they are happy.
Jamaica Gleaner



 Heart Smart Talk
Heart Smart Talk